When you have done the work but applying it still feels inconsistent, additional structured support can help improve engagement, focus, and follow-through over time.
Impact Minds provides Transcranial Magnetic Stimulation (TMS) as part of an integrated system designed to support regulation, improve consistency, and strengthen real-world application.
Licensed Clinical Team • Physician Oversight • Use of evidence-based therapeutic approaches where clinically appropriate • Insurance Accepted
Transcranial Magnetic Stimulation (TMS) is an FDA-cleared, non-invasive, outpatient procedure that uses magnetic pulses to stimulate targeted areas of the brain. It is commonly used for specific conditions such as major depressive disorder when clinically appropriate.
Many individuals explore TMS after putting in consistent effort through counseling, therapy, or other forms of support and still noticing that progress does not hold.
It is common to understand what needs to change, to have strategies in place, and still experience difficulty applying those strategies in real time. This often shows up as hesitation, low energy, difficulty initiating tasks, or inconsistency in follow-through. This gap is not always a lack of effort. It is often a limitation in the systems that support engagement.
TMS may be recommended as part of an individualized treatment plan following clinical evaluation.
TMS is provided within a clinical treatment plan and may be used alongside other services when appropriate. Individual experiences vary, and changes are assessed over time by the clinical team. Over time, this allows strategies that once felt difficult to use to become more available in daily life.
TMS is often provided alongside other clinical services when appropriate. If you are comparing options, you can review a full breakdown here: TMS vs Neurofeedback: What to Know.

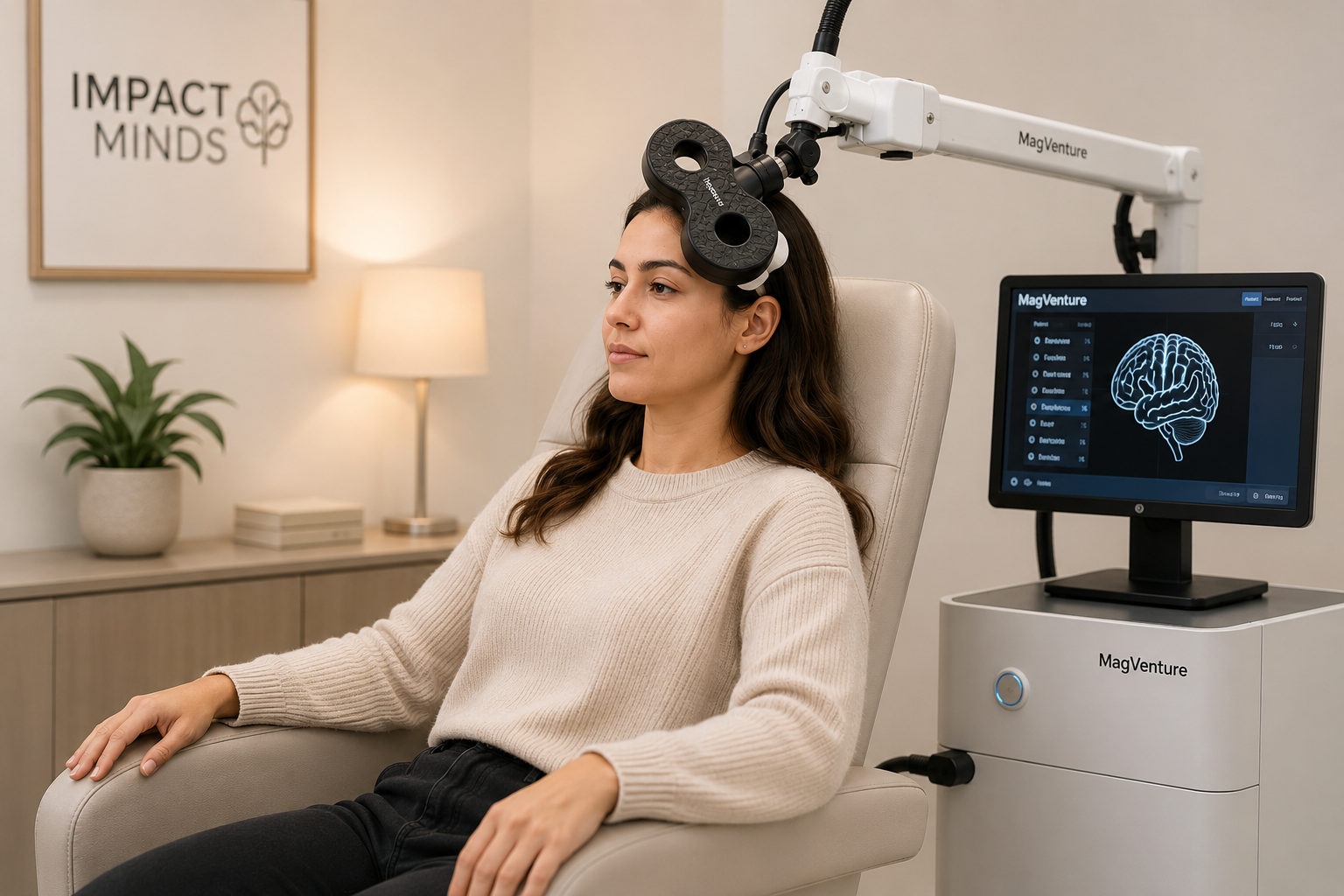
TMS delivers focused magnetic pulses to targeted areas of the brain. These sessions are repeated over time in accordance with established treatment protocols.
The procedure is administered by trained staff under physician supervision. Individual response to treatment varies, and progress is evaluated throughout the course of care.
TMS is used as part of a broader clinical plan when appropriate.
Magnetic pulses target specific brain regions
Sessions are repeated to support sustained change
Treatment is personalized and monitored by licensed clinicians
Have participated in counseling or therapy and want additional structured support
Experience difficulty with follow-through despite understanding strategies
Notice ongoing challenges with focus, engagement, or energy
Have not experienced sufficient progress with other approaches alone
A consultation is used to determine whether TMS is appropriate based on
individual needs and medical considerations.
At Impact Minds, TMS can be provided as a standalone service when appropriate, though it is often integrated into a broader system to support real-world application.
Many individuals already have insight and have developed strategies through counseling or therapy. TMS is introduced to support the ability to apply those strategies more consistently.
Care is structured around four pillars: stability, capacity, control, and ownership. TMS may be incorporated into a clinical treatment plan to support participation in care when appropriate.
This ensures that improvements are not isolated, but connected directly to meaningful action in daily life.

TMS can support initial engagement, making it easier to begin participating in structured care.
As engagement improves, individuals can apply strategies across more situations.
Improved focus supports more intentional responses in real time.
As consistency increases, individuals rely more on their ability to apply skills independently.
TMS may be incorporated into a broader treatment plan when clinically appropriate.
TMS sessions are conducted in an outpatient setting and are typically scheduled multiple times per week over a defined period. Each session involves:

Sessions are monitored by trained staff and overseen by a licensed physician. TMS services are provided under physician supervision and administered by trained clinical staff in accordance with applicable medical and behavioral health regulations.
Most individuals remain awake and alert during sessions and can return to normal activities afterward.
The structure of treatment is designed to provide repetition over time, supporting gradual improvement in engagement and consistency.
Individuals may experience changes in symptoms depending on the condition being treated. Reported experiences can include changes in mood, energy, or overall functioning.
Outcomes vary by individual and are not guaranteed. TMS is used as part of a broader clinical treatment plan when appropriate.
Changes in mood and energy
Improved ability to initiate tasks
Enhanced focus and engagement
At Impact Minds, TMS is integrated within a structured system of care rather than used in isolation.

TMS can support initial engagement, making it easier to begin participating in structured care.
As engagement improves, individuals can apply strategies across more situations.
Improved focus supports more intentional responses in real time.
As consistency increases, individuals rely more on their ability to apply skills independently.
TMS may be incorporated into a broader treatment plan when clinically appropriate.
TMS can be provided on its own or integrated with counseling or therapy. When integrated, it supports a more structured pathway for applying changes in daily life.
While TMS supports regulation and engagement, counseling and therapy provide structure, strategy, and application.
This integration allows individuals to:
Together, this creates a more complete pathway for progress.
Progress with TMS is typically gradual and builds through repetition. While each individual’s experience is different, many people notice changes that develop in stages as engagement improves over time.
PHASE 01
Some individuals begin to notice small shifts in energy, focus, or the ability to initiate tasks. These changes may feel subtle at first, but they often reduce the effort required to begin actions.
PHASE 02
As sessions continue, initiating tasks may feel more manageable. Follow-through becomes more consistent, and strategies developed through counseling or therapy may feel easier to apply in real situations.
PHASE 03
With continued participation, these patterns begin to stabilize. Actions feel more predictable, and responses require less effort to initiate. This supports steadiness across different areas of daily life.
Throughout this process, TMS works best when paired with structured application. As engagement improves, actions become easier to repeat. Repeated actions build consistency. Consistency supports momentum over time.
Changes in ability to initiate or complete tasks
Changes in daily consistency
Changes in focus or attention
Increased engagement in structured activities
Changes in ability to apply learned strategies
Outcomes vary based on individual factors and participation.
Many individuals consider TMS after putting in significant effort and still feeling that progress is inconsistent.
At Impact Minds, TMS is not presented as a separate solution. It is integrated into a system designed to support real-world application at every stage.
This section reflects how that system is experienced.
The same four pillars guide how progress develops, with TMS supporting each one in a practical way:
Sessions are supported by an environment that reduces overwhelm and allows individuals to engage more consistently.
As engagement improves, individuals begin applying strategies across a wider range of situations with less resistance.
Improved focus supports the ability to pause, choose, and respond with intention in real time.
As follow-through becomes more reliable, individuals begin to rely less on external structure and more on their own ability to act.
TMS may be incorporated into a broader treatment plan when clinically appropriate to support participation and engagement in care.
TMS sessions are not isolated from the rest of care. They are experienced alongside counseling, structured activities, and environments designed to reinforce application.
Movement-based engagement supports initiation and follow-through. Structured environments support focus and retention.
Together, these elements create a system where improved engagement leads directly to meaningful action.
As actions become easier to initiate, they begin to feel more manageable. Manageable actions support steadiness. Steadiness supports clarity. Clearer decisions build momentum over time.
This is how TMS becomes meaningful. It can be used on its own, but when integrated into a system, it is more directly connected to real-world application and sustained progress.
No. TMS supports engagement and application but does not replace structured skill development.
Yes. TMS can be provided as a standalone service when appropriate. In some cases, it is also integrated with counseling or therapy to support more structured application of progress.
TMS and neurofeedback are different approaches used within a care plan. TMS uses magnetic stimulation and is a medical service provided following clinical evaluation. Neurofeedback is a training-based approach that focuses on awareness and practicing adjustments through structured feedback. If you are comparing these options, you can read a full explanation here: TMS vs Neurofeedback: What to Know.
You do not have to navigate this alone. If you are considering TMS or want to understand whether it is appropriate for you, a consultation can help clarify the next step.
Free consultations are brief screening calls intended to determine appropriate services and do not constitute a clinical assessment, diagnosis, or medical advice.
If you or someone you know is experiencing a medical or psychiatric emergency, call 911 or go to the nearest emergency room.
For immediate support, contact the 988 Suicide & Crisis Lifeline.
Stronger than yesterday.
We invite you to a new era of mental wellness.
Medical Disclaimer: TMS is a medical procedure provided only after a clinical and medical evaluation to determine appropriateness. Treatment plans are individualized, and outcomes vary. TMS may be used alongside other clinical services when appropriate. Potential risks, benefits, and alternatives are reviewed as part of the informed consent process prior to initiating treatment.